Charcot foot is a disorder that leads to the destruction of joints in the foot. Charcot Foot commonly affects patients in the 50-60 age bracket and about 3% of all people with diabetes. A person who suffers from Charcot’s Foot often loses the sense of pain and positioning. As a result, the foot is unable to respond to abnormal stress subsequently leading to joint collapse and disintegration.
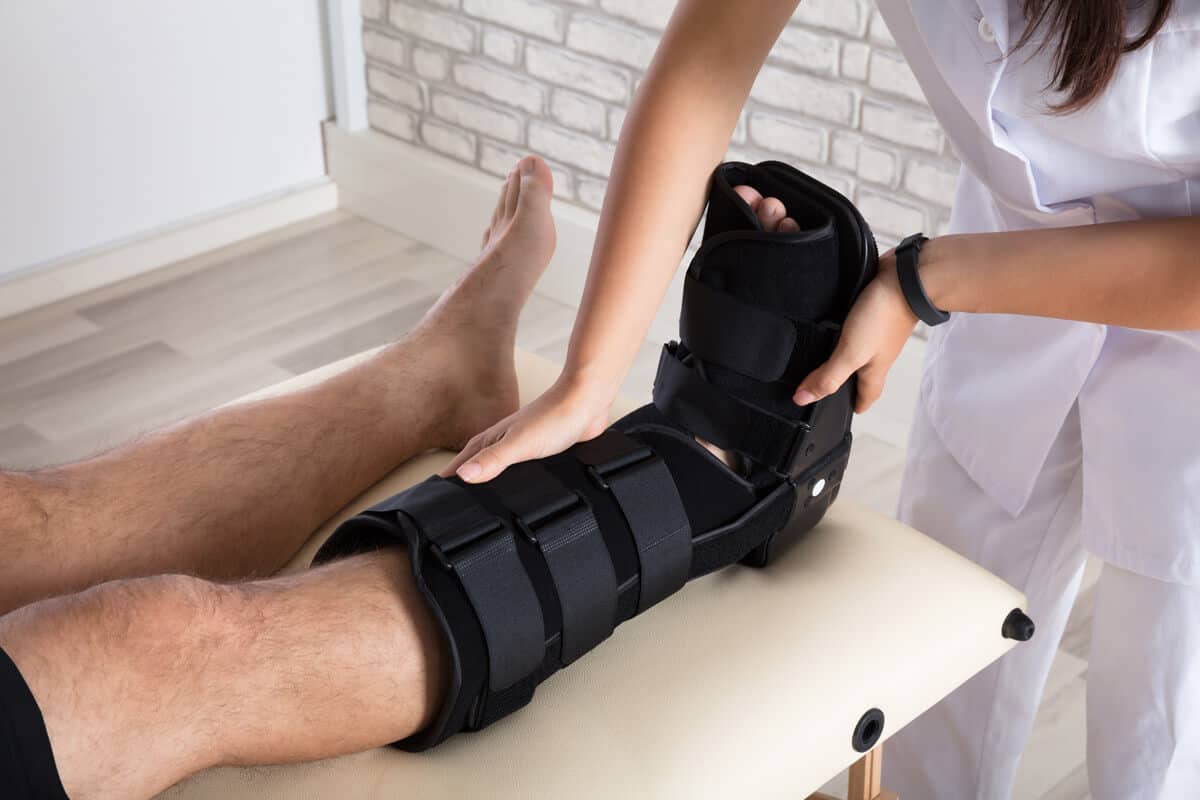
You will notice the following typically on one foot only:
The exact cause of Charcot’s foot is still unknown. There are 2 main theories. The first relates to lack of sensation.
The surgical procedure often involves one or more of the following procedures:
Since most diabetic patients with Charcot’s foot also suffer from poor circulation to the feet, there is a high risk of delayed healing and possible postoperative infection. There is also a possibility of post-operative complications such as:
The key to proper treatment of Charcot Foot is prevention. This could be achieved by visiting your podiatrist for regular screening. Your podiatrist would screen for:
The screening process helps you to be aware of the current condition of your feet. This would indefinitely minimize the risk of suffering from a more severe progression of this disorder.
Ready to give your feet the care they deserve? Book your appointment online or call us and experience our expert podiatry services at any of our six clinic locations.